Foot pain rarely stays local. Because your feet absorb impact and keep you balanced, even a mild strain can change how you walk. That change shifts stress into other areas, so foot problems often show up later as ankle pain, knee strain, hip tightness, or lower back discomfort. The key is understanding what is happening in the foot itself, and what it may lead to if ignored.
Below are 20 common foot issues explained in more detail.
1. Plantar fasciitis
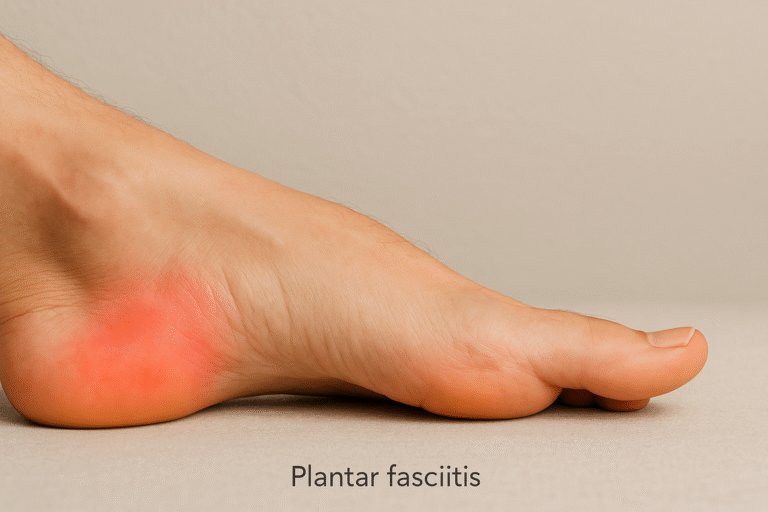
The plantar fascia is a thick fibrous band that supports your arch and helps transfer force during walking. When it is repeatedly overstretched, small tears develop where it meets the heel. This is common in people who stand long hours, walk on hard floors, gain weight quickly, or wear shoes without arch support.
What you feel: stabbing pain under the heel when you take your first steps, then a dull ache later in the day.
What it leads to: limping or altered walking, which can create calf tightness and knee or hip strain over time.
2. Heel spur
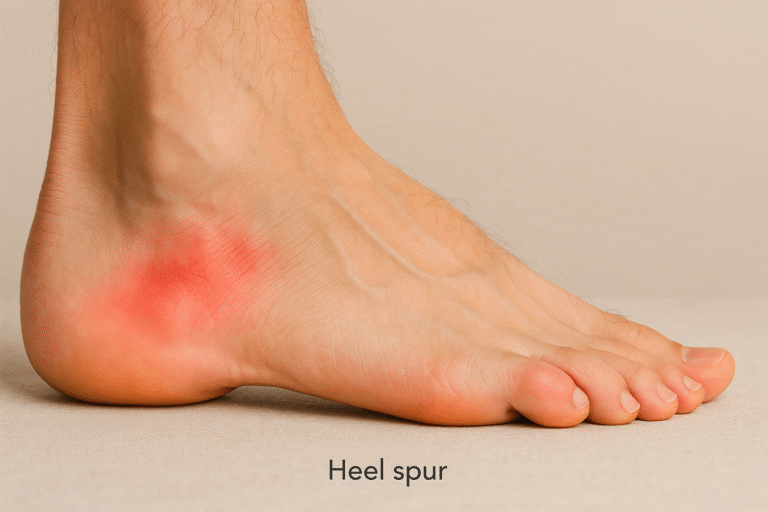
A heel spur forms when the heel bone responds to repeated pulling or pressure by laying down extra calcium. It is not the spur itself that hurts at first, but the irritation it creates in surrounding soft tissue. It often develops alongside plantar fasciitis.
What you feel: deep heel ache that worsens after standing or walking, sometimes sharp if the spur irritates tissue.
What it leads to: long lasting heel sensitivity that does not settle unless pressure patterns are corrected.
3. Achilles tendinitis
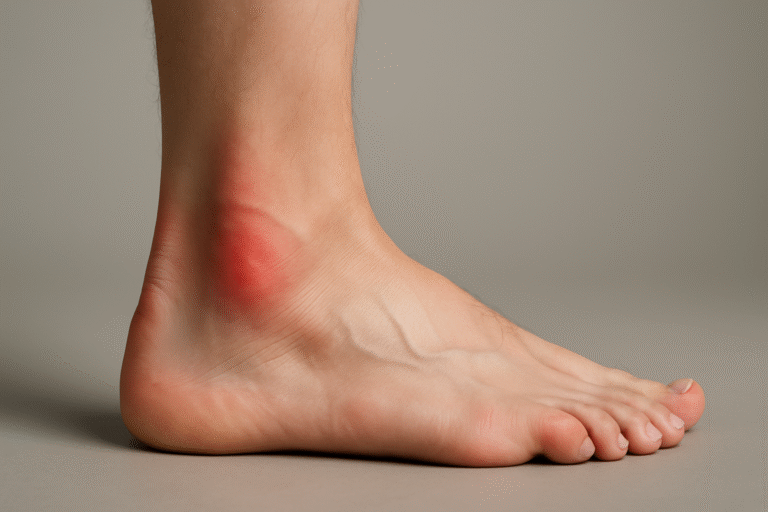
Your Achilles tendon stores and releases force with every step. Overuse, tight calves, sudden increases in walking or running, or an unstable heel position can overload it. Microscopic fibre damage causes thickening and inflammation.
What you feel: soreness or stiffness at the back of the heel, often worse after activity or first thing in the morning.
What it leads to: reduced ankle mobility and higher risk of more serious tendon injuries if activity continues without support.
4. Flat feet or fallen arches
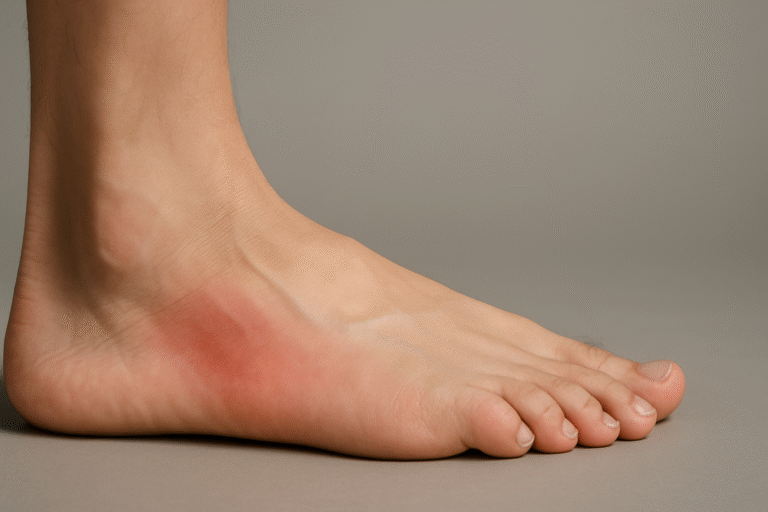
A flat foot means the arch sits low or collapses under weight. It can be present from childhood or develop through ageing, weak foot muscles, ligament laxity, injury, or weight gain. Without an arch, impact is not distributed properly.
What you feel: tired arches, inner ankle pain, soreness after long walking, or aching in the heels.
What it leads to: overpronation and increased strain in ankles, knees, hips, and lower back because the foot loses stability.
5. Overpronation
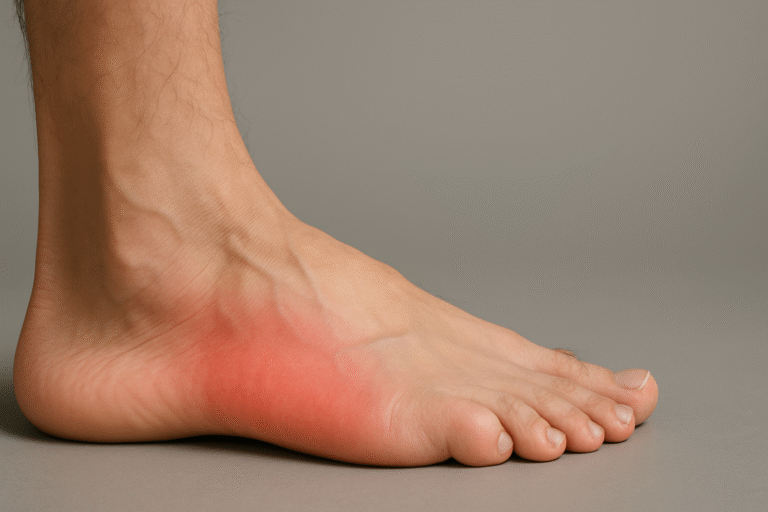
Overpronation is an inward rolling motion that becomes excessive when the arch drops. It is common in flat feet but can also occur with weak ankle control. Each step pushes weight towards the inner foot, changing how force travels through the leg.
What you feel: arch strain, inner heel pain, ankle fatigue, or shin tightness.
What it leads to: inward knee tracking and hip compensation, contributing to recurring foot pain and sometimes lower back discomfort.
6. High arches
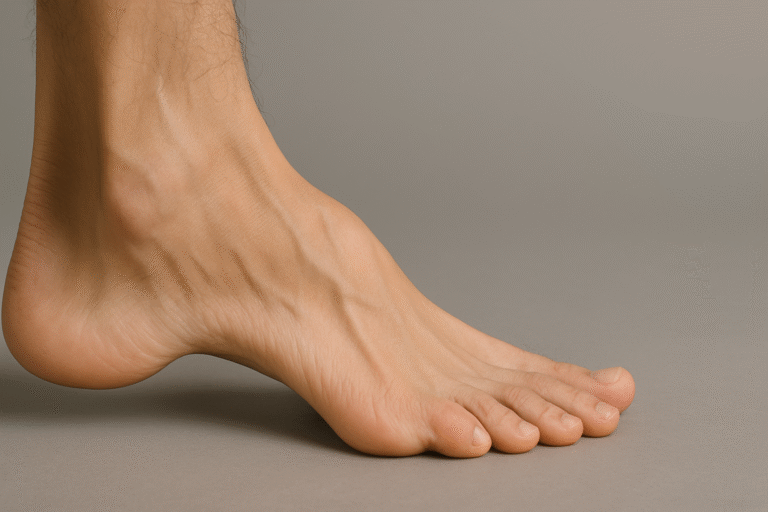
High arches reduce the contact area with the ground. That means pressure concentrates under the heel and ball of the foot instead of spreading evenly. High arches are often inherited, but can also relate to nerve or muscle imbalance.
What you feel: soreness in the heel and forefoot, instability, or frequent ankle sprains.
What it leads to: poor shock absorption and repetitive strain at pressure points.
7. Metatarsalgia
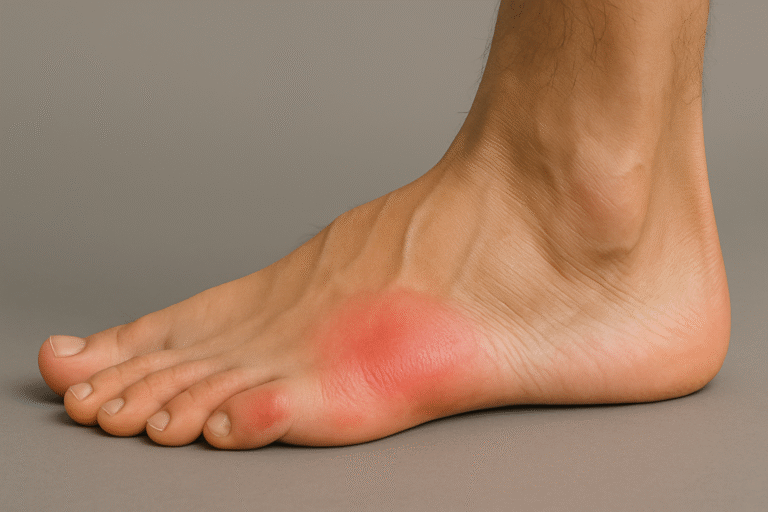
Metatarsalgia develops when the metatarsal heads in the forefoot take repeated overload. Thin soles, high heels, long standing, high impact sport, or weight shift from other deformities can cause it.
What you feel: burning or aching under the ball of the foot, worse after walking or standing.
What it leads to: altered stride to avoid pressure, which may trigger calf, knee, or hip tightness.
8. Morton’s neuroma
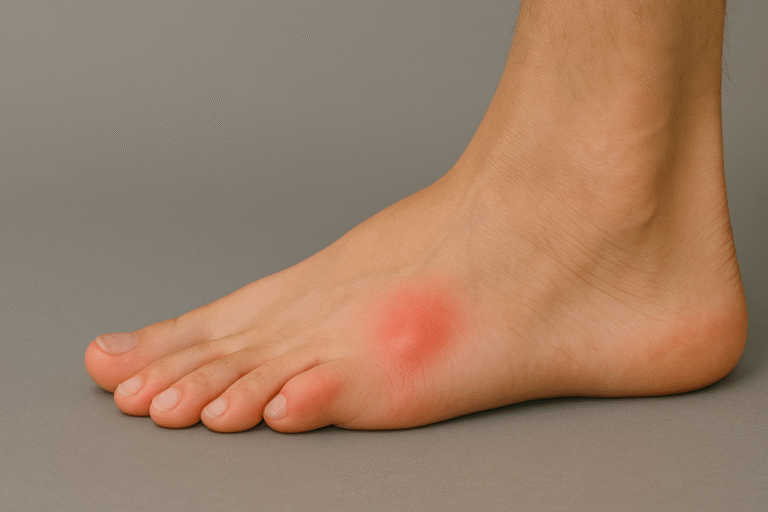
This condition occurs when a nerve between the toes becomes compressed repeatedly. Tight toe boxes, high heels, and constant forefoot pressure trigger thickening around the nerve.
What you feel: sharp burning pain, tingling, or numbness between toes, often feeling like a pebble is stuck in your shoe.
What it leads to: reduced tolerance for walking and footwear, and worsening nerve sensitivity if compression continues.
9. Bunions (hallux valgus)
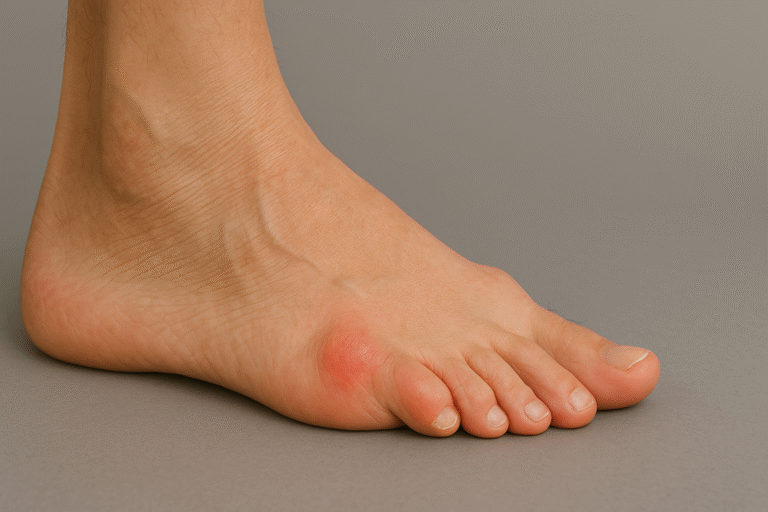
A bunion forms when the big toe joint gradually shifts out of alignment. It is strongly influenced by inherited foot shape. Tight or narrow shoes accelerate the change once it begins.
What you feel: swelling, redness, and aching at the big toe base, especially after long standing.
What it leads to: altered weight bearing that increases ball of foot pain and may crowd other toes.
10. Hammertoes
Hammertoes happen when tendons controlling the toes become imbalanced, pulling the toe into a bent position. This is often triggered by narrow footwear, long term bunion pressure, or muscle weakness.
What you feel: pain on top of the toe from rubbing, and soreness under the ball of the foot.
What it leads to: stiff toes that are harder to straighten, increased corns, and difficulty wearing normal shoes comfortably.
11. Turf toe
Turf toe is a sprain at the big toe joint caused by forceful upward bending. It is common in running, jumping, football, or uneven push off during movement. Ligaments stretch or tear slightly.
What you feel: swelling and sharp pain near the big toe joint, especially during push off.
What it leads to: reduced toe mobility and possible early joint stiffness if reinjury happens repeatedly.
12. Posterior tibial tendon dysfunction
The posterior tibial tendon supports the inner arch. Repeated overload from flat feet, overpronation, or long standing can cause microtears. As it weakens, the arch collapses further.
What you feel: inner ankle pain and arch strain, often worsening through the day.
What it leads to: foot instability and progressive flattening that can become rigid if untreated.
13. Peroneal tendinitis
Peroneal tendons stabilize the outer ankle. They become irritated from uneven terrain, weak ankle control, high arches, or repetitive running.
What you feel: soreness along the outer foot or ankle, especially after activity.
What it leads to: reduced ankle stability and higher risk of sprains if tendon irritation continues.
14. Tarsal tunnel syndrome
A nerve passing through the inner ankle becomes compressed due to swelling, flat foot collapse, injury, or nearby tendon irritation.
What you feel: burning or tingling in the arch and sole, sometimes numbness that worsens after standing.
What it leads to: persistent nerve pain patterns and reduced comfort in daily walking.
15. Stress fractures
Stress fractures form when bone is overloaded faster than it can repair itself. Sudden increases in walking, running, dancing, or carrying weight for long hours are typical triggers.
What you feel: pinpoint sharp pain that becomes worse with standing and settles with rest.
What it leads to: larger fractures if activity continues, making recovery longer.
16. Arthritis in the foot
Arthritis occurs when joint cartilage wears down or becomes inflamed. This can be age related, post injury, or autoimmune. Without cartilage cushioning, joint surfaces rub and swell.
What you feel: stiffness, aching, and swelling in the toes, midfoot, or ankle, worse after rest.
What it leads to: reduced mobility, altered gait, and long term pain flare patterns.
17. Gout
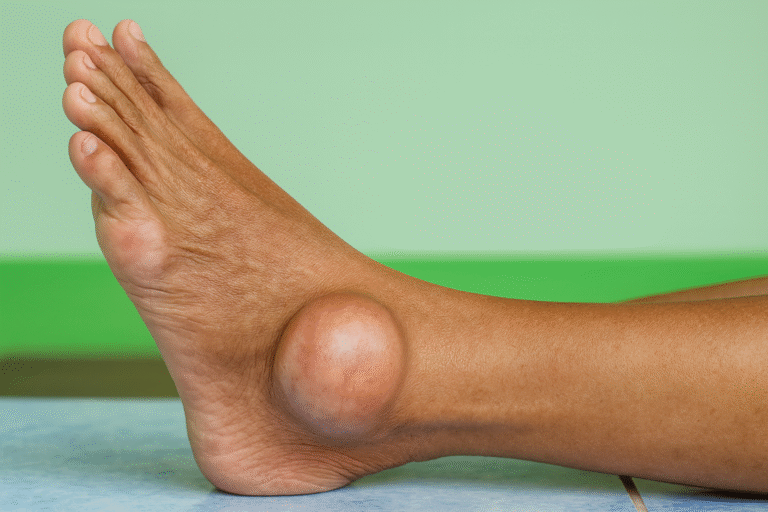
Gout develops when uric acid crystals collect in a joint. It may be linked to diet, dehydration, genetics, or metabolic conditions. The immune system reacts strongly, causing sudden inflammation.
What you feel: severe sharp pain, redness, heat, and swelling in the big toe or other joints.
What it leads to: recurring flare-ups and joint damage if attacks repeat often.
18. Corns and calluses
These are protective skin thickening caused by repeated rubbing or pressure. They often appear because of tight shoes, toe deformities, or uneven weight distribution.
What you feel: tenderness or sharp discomfort when pressure is applied.
What it leads to: cracks, skin breakdown, and worsening pain if the pressure cause is not corrected.
19. Ingrown toenail
This happens when the nail edge grows into skin due to trimming shape, tight footwear pressure, or minor toe injuries. Inflammation builds and bacteria may enter.
What you feel: throbbing tenderness at the nail corner, swelling, and sometimes pus if infected.
What it leads to: difficulty wearing shoes and walking normally, with risk of persistent infection.
20. Blisters
Blisters form when friction separates skin layers, often due to poorly fitting shoes, damp socks, or long walking in heat. The body creates fluid to protect the area.
What you feel: burning pain with each step, especially if the blister is large.
What it leads to: open wounds if it breaks, with infection risk if not cleaned and protected.
Treatment and Management for Foot Pain
Treating foot pain starts with two priorities: calming the irritated area and fixing the pressure pattern that caused it. Many foot problems begin as small overload issues, so early care often prevents them from turning into chronic pain. The right approach depends on the type of foot pain, how long it has been present, and whether alignment issues like flat feet or overpronation are involved.
Treat the root cause, not only the symptom
Once the pain starts to ease, long term improvement comes from correcting what triggered it. Many types of foot pain are caused by uneven loading. If one part of the foot is repeatedly taking more weight than it should, the tissue there stays irritated.
That is why it helps to look at:
- Arch height and stability
- How your ankle rolls during walking
- Whether your shoes allow proper support
- How weight spreads across your foot
- Wear correct shoe size
Fixing these patterns reduces repeat stress and lowers the chance of pain coming back.
Condition focused treatment notes
Different foot pain types respond to different care approaches. Here is the practical direction behind the most common ones:
1. Plantar fasciitis and heel spur pain
These often respond to calf stretching, structured footwear, and arch support. The goal is to reduce pulling on the heel area while the tissue recovers.
2. Achilles tendinitis
This improves with gradual tendon strengthening, calf mobility work, and avoiding sudden jumps in activity volume.
3. Metatarsalgia and Morton’s neuroma
These conditions need reduced pressure on the forefoot. Wide toe box shoes, cushioned soles, and support under the arch can help shift weight away from the painful nerve or bone area.
4. Bunions, hammertoes, corns, and calluses
Footwear that gives toes space and spreads weight evenly matters more than temporary padding alone. The aim is to reduce rubbing and pressure points.
5. Arthritis and gout
First focus is inflammation control. Then long term relief depends on joint stability and footwear that limits stress on stiff or swollen joints.
6. Stress fractures
These need rest and time. If you continue loading the foot early, the crack can worsen and recovery becomes longer.
7. Tarsal tunnel syndrome and nerve based pain
Burning or tingling suggests nerve irritation. Reducing pressure and correcting foot alignment early helps prevent worsening symptoms.
How Custom Insoles Can Help
A major link between many foot conditions is uneven pressure and weak arch support. When one area takes excess weight repeatedly, tissue becomes irritated, nerves are compressed, or bones overload. Custom insoles reduce that by supporting the arch, stabilising pronation or supination, and spreading pressure more evenly.
The Insole Company creates custom insoles using a detailed 2D and 3D foot scan that maps your arch profile and pressure points. This allows the insole to match your foot mechanics rather than using a generic mould. People with flat feet, overpronation, high arch, supination, plantar fasciitis, heel pain, forefoot strain, or fatigue from long standing often benefit from that customized support book your appointment to get your scan done and find the right insole for your feet.
Key Takeaway
Foot pain may begin in one small area, but it often reflects pressure and alignment problems across the whole foot. When you understand how a condition develops and what it leads to, treatment becomes far more effective. Proper footwear and custom insoles can reduce stress, improve comfort, and stop the cycle before pain spreads further.