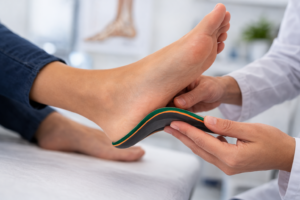
If you live with diabetes, looking after your feet is absolutely vital. A diabetic foot is more vulnerable to problems such as ulcers, foot sores, infections and long-lasting pain. High blood sugar levels can damage nerves and reduce blood flow to the feet, which means that even a small blister or area of rubbing can turn into a serious issue if it is ignored.
This is where diabetic insoles, custom orthotics come into play. These special inserts are designed to protect the feet, ease diabetic foot pain and make every step more comfortable.
What Are Diabetic Insoles?
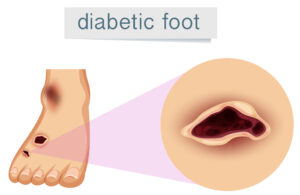
Diabetic insoles are specially designed inserts that sit inside your shoes and give your feet extra protection, cushioning and support. They are made for people with diabetes, whose feet may be more vulnerable to problems such as ulcers, calluses and pressure points.
What Do Diabetic Insoles Do?
- Provide gentle but consistent cushioning under the whole foot to reduce impact when you walk.
- Help distribute body weight more evenly, so one small area of the foot is not taking all the pressure.
Why Diabetic Feet Need Extra Care
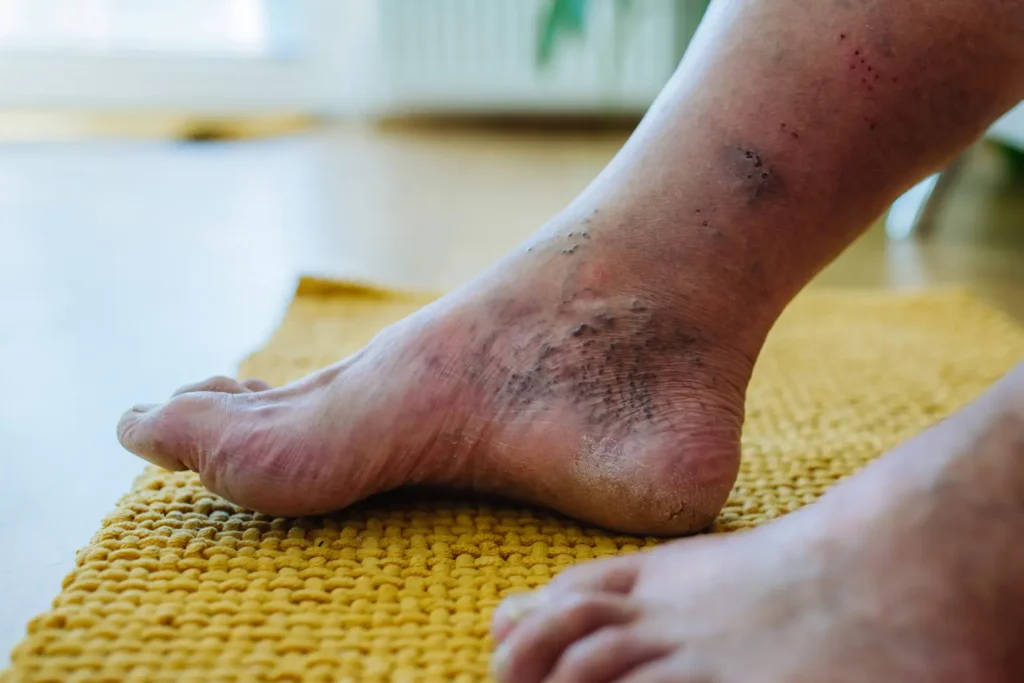
Image Courtesy: thefootpractice.com
A person with diabetes may develop two main problems that affect the feet:
1. Nerve damage (neuropathy)
When the nerves are damaged, you may notice tingling, burning or complete numbness. This means you might not feel a cut, blister or stone in your shoe. Because you do not feel pain, you continue to walk on the injury and it gradually becomes worse. This is a common pathway to ulcers in the diabetic foot.
2. Poor circulation
Diabetes can narrow and stiffen the blood vessels that supply the legs and feet. With less blood flow, wounds take longer to heal, the skin becomes fragile and the risk of infection increases.
Because of this combination of reduced feeling and slower healing, everyday pressures from footwear become a much bigger issue. That is why finding a good shoe insole can make a real difference in long-term foot health.
Here is how diabetic insoles help.
1. Reduce friction and rubbing inside the shoe, which lowers the risk of blisters and skin breakdown.
2. Often use moisture-wicking and breathable materials to keep the foot drier and more comfortable.
3. Unlike standard insoles that focus mostly on comfort, diabetic insoles are designed specifically to protect high-risk feet and to support long-term foot health in people with diabetes.
Key Benefits Of Diabetic Insoles
Good quality diabetic insoles offer several important protective features. Below are the main benefits, explained in more detail.
1. Pressure Redistribution
Each step you take puts pressure on different parts of your feet. Without support, certain areas, such as the ball of the foot or the heel, may carry too much weight. Excessive pressure leads to calluses, corns and eventually ulceration.
Diabetic insoles are designed to spread the load more evenly. Instead of one small area taking all the stress, the insole uses its contours and cushioning to move pressure across a wider surface. This is a fundamental part of foot sores treatment and prevention.
2. Shock Absorption
Walking on hard surfaces sends impact forces up through your heels and arches. For someone with neuropathy, these repeated shocks can damage the skin and tissues, even if there is little or no pain at the time.
Diabetic insoles are made with materials that absorb and soften each step. This shock absorbing layer protects fragile tissues and can ease diabetic foot pain, as well as general heel and arch pain such as plantar fasciitis.
3. Diabetic Arch Support And Alignment
Many people with diabetes also have issues with foot posture. The arches may roll inwards too much or be unusually high. Poor alignment alters the way pressure is distributed across the foot.
Specialised diabetic arch support inside insoles encourages the foot into a healthier position. By supporting the arch correctly, the insole:
1. Reduces strain on ligaments and tendons.
2. Helps the ankle and knee line up better.
3. Minimises the development of pressure points that later turn into sores.
4. Moisture And Temperature Management
Diabetic feet often benefit from a stable, dry environment. Excess moisture softens the skin and makes it more vulnerable to damage, while cold feet are a common discomfort for people with circulatory problems.
Many diabetic insoles use fabrics that wick sweat away from the skin and allow air to circulate inside the shoe. Some designs also provide a light insulating effect that can help with diabetes cold feet treatment, keeping feet comfortably warm without overheating
At The Insole Company, our specialized diabetic insoles are designed to reduce the risk of ulceration and callus formation and promote even weight distribution across the whole foot. They provide a total contact fit that follows the natural contours of your feet, precise offloading in vulnerable areas, enhanced cushioning for daily comfort, and are made from lightweight, breathable materials to help keep your feet cool and dry.
If you are living with diabetes and have noticed any changes in your feet, or you have been advised that you are at higher risk of ulceration, our insole specialists at The Insole Company can help. Book an appointment with our team to discuss whether custom orthotics and diabetic insoles are suitable for you and to receive tailored advice on protecting your feet long term.
Diabetic Insoles Vs Diabetic Shoes
Many people wonder whether they should invest in diabetic shoes, insoles or both. The answer depends on your current footwear and the condition of your feet.
Diabetic Insoles
Most Popular
Diabetic Insoles
₹5,000+
Reduces risk of ulceration and callus formation. Promotes even weight distribution
-
Total contact fit -
Precise offloading -
Lightweight and breathable -
Enhanced cushioning -
Medical Grade TPU Foam
Diabetic insoles are ideal if you:
1. Already own good quality, well-fitting shoes.
2. Want to enhance cushioning and support without replacing all your footwear.
3. Need targeted protection in specific areas such as the heels or balls of the feet.
They can be moved between different pairs of shoes, as long as there is enough depth and space.
Diabetic Shoes/Sandals
Diabetic shoes are specially designed footwear for people with diabetes. They usually have:
1. Extra depth and width to allow for swelling and deformities.
2. Seamless interiors so there are no rough seams to rub against the skin.
3. Soft, breathable materials and supportive soles.
Many diabetic shoes include their own insoles. Others are designed so that custom orthotics or diabetic inserts can be placed inside. They are particularly helpful for those with significant deformity, recurrent ulcers or difficulty finding comfortable shoes on the high street.
Managing Diabetic Foot Pain With Insoles
Diabetic foot pain can come from several sources, including nerve damage, joint strain and pressure from footwear. The right insoles can play a big part in easing this discomfort.
They do this by:
- Supporting the arch and heel so that joints are not overloaded.
- Reducing impact forces that aggravate painful areas.
- Improving alignment so muscles and ligaments are under less stress.
It is important to remember that insoles are one part of a wider foot sores treatment and diabetic foot care plan. They work best alongside regular podiatry checks, good blood sugar control and daily self-inspection of the feet.
Practical Tips For Using Diabetic Insoles
To get the most benefit from your insoles or orthotics:
1. Choose suitable footwear
Your shoes should have enough room for both your foot and the insole. Avoid styles that are too tight across the toes or too shallow in depth.
2. Check your feet every day
Look for redness, hard skin, cracks or blisters. If you have reduced sensation, use a mirror or ask someone to help you check the soles.
3. Introduce new insoles gradually
Wear them for a few hours at first and slowly increase the time. This allows your feet, ankles and legs to adjust to the new support.
4. Replace worn insoles
Over time, materials compress and lose their shock-absorbing ability. If your insoles look flat, torn or feel less supportive, it may be time for a new pair.
5. Keep regular appointments
Arrange routine reviews with a podiatrist or healthcare professional. They can assess how well your insoles are working and make adjustments if necessary.
Conclusion
For anyone living with diabetes, the right combination of diabetic insoles, custom orthotics and supportive footwear can make a real difference to comfort and long-term foot health. Always speak to your podiatrist or healthcare provider to find the most suitable option for your needs. If you would like personalised guidance and fittings, book an appointment with our insole team to get expert support for your feet.