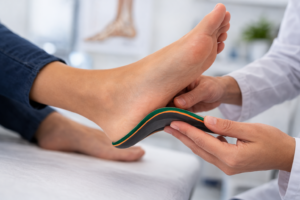
If you have diabetes, should you invest in diabetic shoes or are diabetic insoles enough? The wrong choice can increase the risk of ulcers and long-term foot damage.
Foot complications are among the most common and preventable issues in diabetes. Reduced sensation, poor circulation, and delayed healing make proper footwear essential. Diabetic shoes and diabetic insoles both play important but different roles in protecting sensitive feet.
Understanding the difference can help you choose the right level of protection for your condition.
What Are Diabetic Shoes?
Diabetic shoes are medical-grade footwear designed specifically for people with diabetes. Unlike standard shoes, they are constructed to protect sensitive feet and accommodate changes in foot shape that often occur over time.
These shoes typically feature a deeper and wider toe box, allowing the toes to sit naturally without compression. The interior is seamless, which significantly reduces friction and the risk of skin irritation. Materials are chosen to promote airflow and moisture control, helping to maintain a healthier skin environment.
From a clinical perspective, diabetic shoes are often recommended for individuals with advanced neuropathy, foot deformities, or a history of ulcers.
What Are Diabetic Insoles?
Diabetic insoles are specialised inserts worn inside shoes to manage pressure and improve weight distribution across the foot. They are commonly prescribed as part of a preventative or early-stage intervention strategy.
These insoles are manufactured using soft, multi-layered materials that adapt to the foot’s contours. This allows pressure to be spread more evenly, reducing stress on high-risk areas such as the ball of the foot and heel. Many designs also incorporate antimicrobial properties to reduce infection risk.
Diabetic insoles can be worn inside diabetic shoes or, in some cases, inside appropriately fitted everyday footwear.
Diabetic Shoes vs Diabetic Insoles: Key Differences
| Aspect | Diabetic Shoes | Diabetic Insoles |
|---|---|---|
| Primary Purpose | Complete protective footwear solution | Pressure redistribution and cushioning inside shoes |
| Design Focus | Seamless interior, extra depth, wide toe box | Soft multi-layer cushioning and pressure relief |
| Level of Protection | High – protects from external friction and internal pressure | Targeted – mainly reduces underfoot pressure |
| Customisation | Limited to size, depth and width | High – can be custom-moulded and clinically adjusted |
| Can They Be Used in Regular Shoes? | No – they replace regular footwear | Yes – can be worn inside properly fitted everyday shoes |
| Which Is More Expensive? | Generally more expensive due to full shoe construction | Typically more affordable unless custom-made |
| Doctor Recommendation | Recommended for advanced neuropathy, deformities, ulcer history | Recommended for early-stage risk, prevention and mild neuropathy |
| Better for Ulcer Prevention? | Best for high-risk patients and recurring ulcers | Effective for pressure reduction in mild to moderate risk cases |
| Need for Additional Footwear? | No | Yes |
| Best Suited For | Severe or high-risk diabetic foot conditions | Prevention, mild symptoms and pressure sensitivity |
Which Diabetic Foot Conditions Are Better Managed With Insoles or Shoes?
Diabetic insoles are suitable for:
-
Mild neuropathy without skin breakdown, where pressure relief is needed but structural support remains adequate.
-
Generalised foot pain or early callus formation caused by uneven pressure distribution.
-
Conditions like metatarsalgia or plantar fasciitis requiring cushioning and load redistribution.
-
Preventative care in patients with good skin integrity but increased risk of pressure-related injury.
Diabetic shoes are recommended for:
-
A history of foot ulcers or recently healed wounds requiring maximum protection.
-
Severe neuropathy or significant loss of sensation increasing ulcer risk.
-
Structural deformities such as hammer toes or Charcot foot that need external support.
-
Persistent pressure areas or swelling that cannot be managed with insoles alone.
The Role of Custom Insoles in Diabetic Foot Care
Custom insoles play an important role in diabetic foot care when they are properly prescribed and clinically designed. Unlike standard or off-the-shelf inserts, custom insoles are created based on an individual’s foot shape, pressure patterns, and gait mechanics, allowing targeted pressure redistribution while maintaining overall stability.
Although they can support joint alignment and improve lower-limb biomechanics, alignment is never the primary objective in diabetic patients. The main clinical priority remains reducing pressure and protecting the skin from breakdown.
When designed correctly, custom insoles achieve this balance without introducing new pressure points, making them particularly suitable for individuals with uneven load distribution, early deformities, or increased risk of ulceration. Regular review is essential, as changes in foot structure or sensation may require timely adjustments.
Clinical Advice for Diabetic Foot Protection
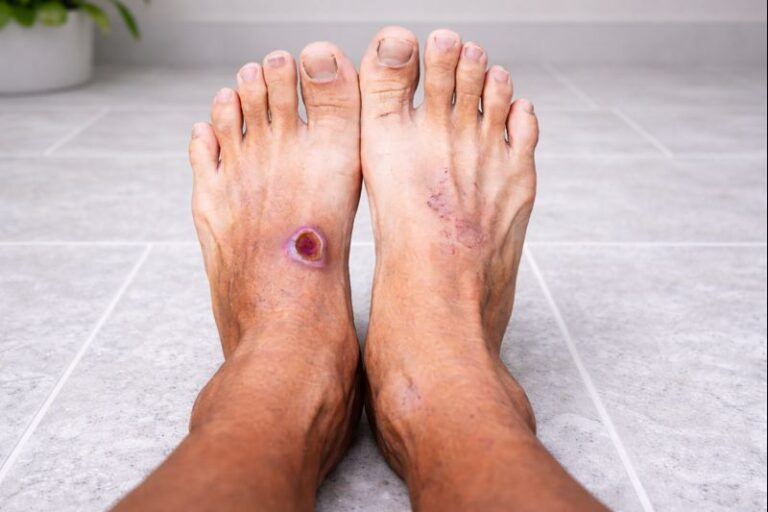
Footwear decisions should never be made in isolation. A podiatric or orthopaedic assessment can identify pressure points, gait abnormalities, and footwear risks before complications arise. Regular foot checks and timely adjustments remain the cornerstone of diabetic foot care.
FAQs
1. Are diabetic insoles enough to prevent ulcers?
Diabetic insoles help reduce pressure and friction, but high-risk patients may still require protective diabetic shoes for full ulcer prevention.
2. Can I wear diabetic insoles in normal shoes?
Yes, provided the shoes fit properly and offer adequate depth to accommodate the insole without creating pressure.
3. Are custom diabetic insoles better than ready-made ones?
Custom insoles are generally more effective because they are designed to match individual pressure patterns and foot structure.
4. How often should diabetic insoles be replaced?
Most diabetic insoles should be reviewed every 6–12 months, or sooner if wear, compression, or foot changes occur.
5. Do diabetic shoes cure neuropathy?
No, diabetic shoes do not treat neuropathy but help reduce injury risk by protecting insensitive feet.
Conclusion
Diabetic shoes and diabetic insoles serve different levels of risk. One provides full protection, while the other offers targeted pressure relief. Choosing the right option at the right stage helps prevent ulcers and protect mobility.
At our clinic, we design clinically tailored diabetic insoles to reduce pressure and support sensitive feet. Book an appointment to determine the safest solution for your needs.